Case of the Month ...
Case History
45 years old African American male presented with a right-sided neck mass for about a year. It had changed in size slightly from time to time, but generally had not completely gone away. It had never been painful and there had never been inflammation of the overlying skin or any drainage. He was basically, completely healthy otherwise. Physical examination revealed a large, right-sided parotid mass, measuring about 5 cm in diameter and involving most of the parotid gland. It was nontender and there was no inflammation of the overlying skin. The facial nerve worked normally. A fine needle aspiration biopsy was performed. (Figure 1-2)
Diagnosis & Discussion
click on image for larger version
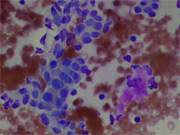
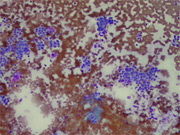
Figure 1
Cytologic Diagnosis: Epithelial neoplasm with basal cell features, differential diagnosis included basal cell adenoma, and adenoid cystic carcinoma.
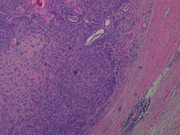
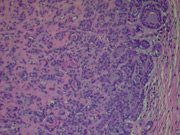
The patient subsequently underwent total parotidectomy with facial nerve preservation. (Figure 3-4)
Histologic Diagnosis: Basal cell adenoma with tubular, trabecular, and membranous patterns.
Discussion: Basal cell adenoma is now recognized as a separate entity in the most recent classification of salivary gland tumors by the World Health Organization.
Majority of these tumors arise in the parotid gland of elderly patients. Microscopically, the tumor cells palisade and form solid trabecular or tubular structures. These architectural formations are surrounded by a well-defined basement membrane. The stroma may be quite vascular but does not have the myxochondroid quality seen in pleomorphic adenoma.
The aspirates from basal cell adenoma are usually cellular and consist of a monomorphic population of basaloid cells arranged in cohesive large tissue fragments with irregular branchings, smaller clusters and cords as well as single cells. Cellular palisading at the periphery of the clusters has been reported. Individual tumor cells have small, uniform, oval nuclei with fine chromatin and inconspicuous nucleoli. They often appear as naked nuclei or have scant cytoplasm, resulting in a high nuclear to cytoplasmic ratio. Basal cell adenomas may demonstrate variable amounts of metachromatic basement membrane-like material , mimicking a cellular pleomorphic adenoma. Other cell types such as hyaline cells and spindle-shaped cells commonly seen in pleomorphic adenoma are usually not present in basal cell adenoma. The finding of classic hyaline globules, similar to those seen in adenoid cystic carcinoma, is a rare finding. The lack of conspicuous cytologic atypia such as prominent nucleoli and mitotic activity makes a diagnosis of basal cell adenocarcinoma less likely. The presence of dyskeratotic squamous cells should raise the suspicious of basaloid squamous cell carcinoma.
Because of its rarity and overlapping of features with other primary salivary gland neoplasms, a specific cytologic diagnosis of basal cell adenoma is difficult. Less than 70% of basal cell adenomas were correctly diagnosed and 17% were interpreted as suspicious or positive for a malignant neoplasm such as adenoid cystic carcinoma. Distinguishing this cytologically from other forms of adenomas is not clinically relevant because the treatment is the same. What is important though is the recognition of the benign nature of this tumor.
References:
Seifert G: Histological Typing of Salivary Gland Tumors. WHO International Histological Classification of Tumours. Berlin , Springer-Verlag, 1991
Huvos AG, Paulino AFG: Salivary Glands, in Sternberg SS (ed). Diagnostic Surgical Pathology, 3 rd Ed. Philadelphia, PA, Lippincott Williams & Wilkins, 1999; 853-884
Klijanienko J, El-Naggar AK , Vielh P: Comparative cytologic and histologic study of fifteen salivary basal-cell tumors: Differential diagnostic considerations. Diagn Cytopathol 1999;2:30-34
Layfield LJ: Fine needle aspiration cytology of a trabecular adenoma of the parotid gland. Acta Cytologica 1985;29:999-1002
Hruban RH, Erozan YS, Zinreich SJ, Kashima H:. Fine-needle aspiration cytology of monomorphic adenomas. Am J Clin Pathol 1988;90:46-51
- Stanley MW, Horwitz CA , Rollins SD , et al: Basal cell (monomorphic) and minimally pleomorphic adenomas of the salivary glands. Distinction from the solid (anaplastic) type of adenoid cystic carcinoma in fine-needle aspiration. Am J Clin Pathol 1996;106:35-41
Acknowledgement: This case is contributed by David Chhieng, M.D. from the Department of Pathology, University of Alabama , Birmingham AL .